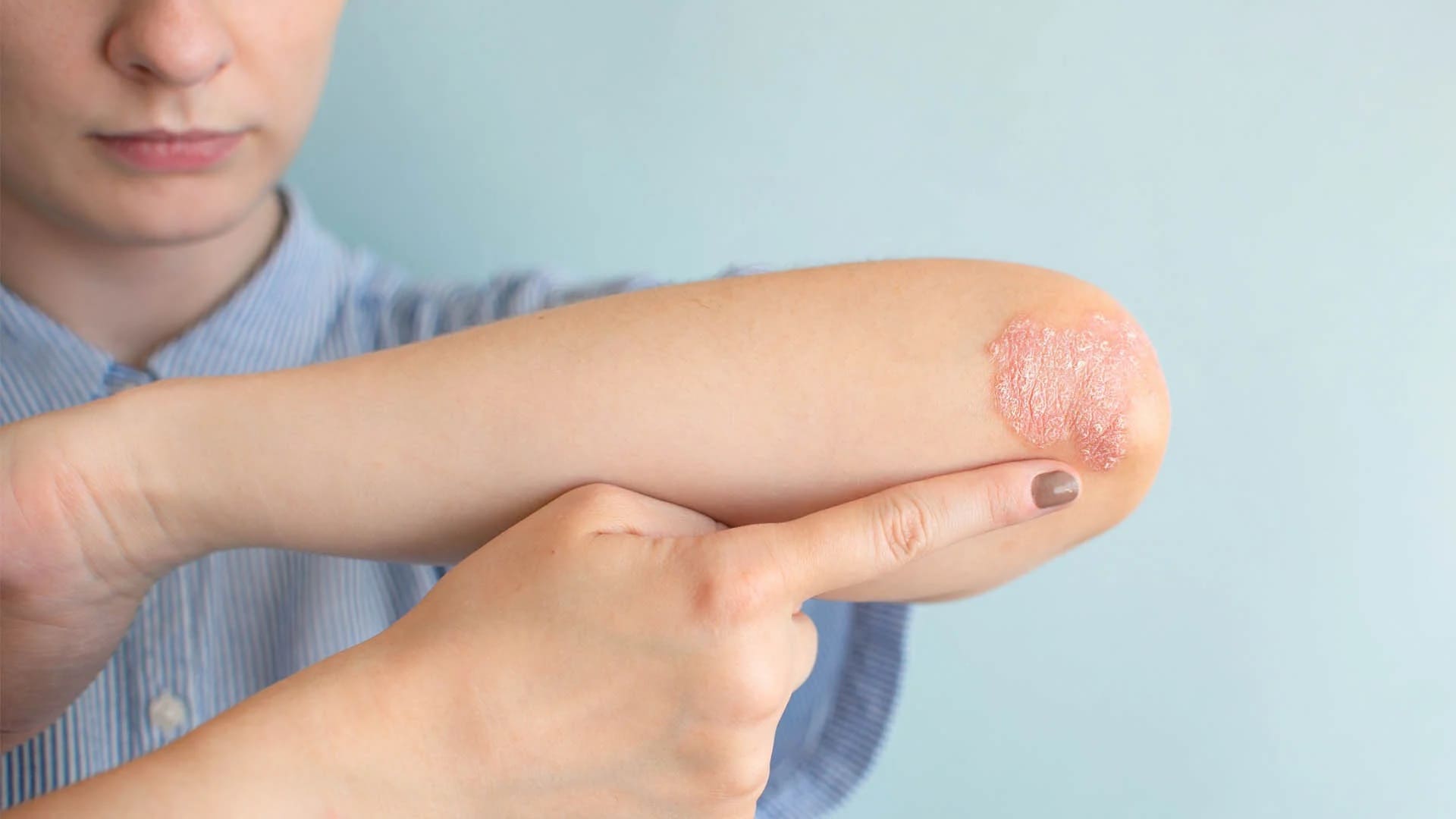
Inverse Psoriasis: Psoriasis is a common autoimmune skin condition that causes skin cells to build up rapidly on the surface of the skin, forming itchy, painful plaques and scales. While psoriasis can occur anywhere on the body, inverse psoriasis presents unique symptoms and challenges.
What Is Inverse Psoriasis?
Inverse psoriasis, also known as flexural or intertriginous psoriasis, occurs in the folds of the skin. This includes areas like the armpits, groin, under the breasts, and around the genitals. The name “inverse” comes from the fact that, unlike plaque psoriasis which builds up on the surface of the skin, inverse psoriasis sinks into the skin folds and has a smooth, inflamed appearance.
While psoriasis vulgaris (plaque psoriasis) is the most common form, inverse psoriasis accounts for about 10-20% of psoriasis cases. Let’s explore the causes, symptoms, and current treatment options for managing this sensitive form of psoriasis.
What Causes Inverse Psoriasis?
The exact cause of inverse psoriasis is unknown, like other forms of psoriasis. However, researchers believe it is an immune system problem that causes skin cells to regenerate too quickly. In a healthy person, skin cells mature and fall off the body over about a month. With inverse-psoriasis, the cell cycle speeds up, taking only about 3-6 days from new cell creation to shedding.
This rapid turnover causes a buildup of skin cells that causes the characteristic red, inflamed lesions. While we don’t know exactly what triggers this immune response, researchers believe inverse psoriasis flares are caused by a combination of genetic and environmental factors.
Genetic Factors
Having a family history of psoriasis increases your risk. Around 40% of people with inverse psoriasis have a close family member with psoriasis. Certain genes like HLA-B13, HLA-B17, HLA-B27, HLA-Cw6, and HLA-DR7 may be inherited and increase psoriasis risk.
Environmental Triggers
Things like stress, skin injuries, infections, and reactions to certain medications can trigger inverse psoriasis flares. The location of skin folds also creates a warm, moist environment that promotes skin cell growth. Friction and sweating can further aggravate lesions.
Symptoms of Inverse Psoriasis
Inverse psoriasis presents differently than other forms of psoriasis because of its location in skin folds and creases. Common symptoms include:
- Smooth, red lesions: Instead of scaly plaques, inverse psoriasis appears as smooth, red, inflamed areas of skin.
- Pain and discomfort: The constant friction and moisture in skin folds make lesions prone to cracking and bleeding. This can cause pain, stinging, and discomfort.
- Itching: Like other forms of psoriasis, inverse psoriasis lesions are often very itchy. Scratching can worsen inflammation and discomfort.
- Increased skin infections: The warm, moist folds of skin create an environment ideal for fungal and bacterial infections like jock itch or yeast infections.
- Lesions in skin folds: Common areas include armpits, under the breasts, groin and genitals, and around the buttocks and anus. Lesions can appear singly or affect multiple areas.
Because of its sensitive locations, inverse psoriasis can have a significant impact on quality of life. It may cause issues with movement, sexual activity, hygiene, and self-confidence. Seeking treatment can help manage symptoms and improve comfort.
Diagnosing Inverse Psoriasis
Inverse psoriasis is often diagnosed simply by physical examination, appearance, and location of the lesions. The smooth, shiny plaques in skin folds are fairly distinctive.
Your doctor may also take a skin sample (biopsy) or scrape some skin cells (skin scraping) to examine under a microscope. This can help rule out other skin conditions like eczema, yeast infections, or bacterial infections that may look similar.
Tell your doctor if you have a family history of psoriasis or if symptoms worsen after infections, stress, or taking certain medications. Your medical history provides important clues in making an accurate inverse psoriasis diagnosis.
Treatment Options for Inverse Psoriasis
While there is no cure for psoriasis, the right treatments can help control inverse psoriasis flares. Because lesions develop in sensitive areas, treatment focuses on reducing inflammation and discomfort. Options may include:
Medicated Ointments and Creams
Over-the-counter creams like hydrocortisone can help reduce mild itching and swelling. Prescription topical treatments contain stronger medications like steroids (clobetasol, triamcinolone), Vitamin D analogs (calcipotriene, calcitriol), or retinoids (tazarotene). These help slow skin cell turnover and reduce plaques and inflammation.
It’s critical to use appropriate strength topical treatments, especially on delicate genital areas. Work closely with your dermatologist to find creams that are effective yet safe for your symptoms and affected areas.
Light Therapy
Phototherapy uses ultraviolet light to treat areas of affected skin. Handheld UVB lamps allow you to target psoriasis plaques while sparing healthy skin. For severe inverse psoriasis, your doctor may recommend full-body UV treatment in an office light booth.
Always protect your eyes and unaffected skin during light therapy. Talk to your dermatologist about risks and ideal treatment schedules.
Systemic Medications
For moderate to severe inverse psoriasis, oral or injectable medications can treat the immune response itself. This helps clear lesions from both visible and covered areas of skin. Options include:
- Biologics: Injectable monoclonal antibodies like Humira (adalimumab), Skyrizi (risankizumab), and Stelara (ustekinumab) target specific parts of the immune response.
- Oral drugs: Medications like Otezla (apremilast), Tremfya (guselkumab), and systemic steroids help regulate immunity and skin cell production.
- Retinoids: Oral retinoids like soriatane help normalize skin cell turnover. Use requires close monitoring for side effects.
While very effective, systemic psoriasis drugs also affect the rest of your immune system. Work with your doctor to weigh the benefits and risks.
Natural and Lifestyle Remedies
Certain natural and self-care approaches may also help soothe inverse psoriasis:
- Moisturize regularly with fragrance-free creams to reduce cracking and itching.
- Avoid triggers like friction, sweating, and skin injuries when possible.
- Wear loose, breathable clothing. Avoid irritating fabrics like wool.
- Gently clean lesions with mild soap and lukewarm water. Avoid harsh scrubbing.
- Manage stress through exercise, meditation, counseling, or other relaxation techniques.
- Consider eliminating possible trigger foods like gluten, dairy, or nightshades if you notice a connection between flares and diet.
While not a substitute for medical treatment, lifestyle measures can be a helpful complement. Work with your doctor to find the right balance of treatments.
Outlook for Inverse Psoriasis
Inverse psoriasis is a lifelong condition. Periods of remission may alternate with unpredictable flares. While not curable, today’s treatments offer a much better quality of life than in decades past.
With an individualized treatment plan, most people achieve significant clearing of inverse-psoriasis plaques. Medications, phototherapy, and lifestyle changes help manage outbreaks and keep symptoms under control.
New biological drugs and improved phototherapy devices continue to advance treatment options as well. With your dermatologist’s help finding the right therapies, you can keep inverse-psoriasis from interfering with your comfort, relationships, and activities.
Frequently Asked Questions About Inverse Psoriasis
Here are answers to some common questions about this sensitive form of psoriasis.
Is inverse psoriasis contagious?
No, psoriasis is not contagious. You cannot spread inverse psoriasis to other people through touch, personal items, or sexual contact. It is an autoimmune condition triggered internally.
How is inverse psoriasis diagnosed?
Doctors usually diagnose inverse psoriasis through physical examination of the characteristic lesions in skin folds, along with your medical history. In uncertain cases, they may take a skin biopsy to confirm.
What is the best over-the-counter inverse psoriasis treatment?
For mild inverse psoriasis, over-the-counter hydrocortisone cream helps reduce itching and swelling. Moisturizers and bath oils can also soothe irritated skin. See your dermatologist if OTC treatments are not keeping flares under control.
When should you see a doctor for inverse-psoriasis?
See your doctor if inverse psoriasis is not controlled with OTC treatments if it affects your day-to-day activities, or if you experience severe itching or pain. Prompt medical treatment can help prevent symptoms from worsening.
What is the most effective prescription treatment for inverse psoriasis?
Powerful topical steroids like clobetasol are usually the first line of prescription treatment. Phototherapy and systemic medications like biologics offer additional options for more stubborn cases. Your dermatologist will help determine the most effective treatment for your symptoms.
Conclusion
The location of lesions in sensitive skin folds makes inverse-psoriasis especially prone to discomfort and social stigma. While symptoms can be frustrating, today’s medical therapies offer safe and effective ways to control flare-ups and improve quality of life.
Work closely with your dermatologist to find an appropriate treatment regimen based on the severity of your inverse-psoriasis. Consistent treatment, along with gentle skin care and avoiding triggers, can help manage this chronic condition.
With the latest therapies, most people achieve significant improvement within a few weeks. You can expect long stretches of clear, comfortable skin with only periodic flares requiring extra treatment. Don’t hesitate to explore both medical and natural options that allow you to confidently manage inverse psoriasis.
Disclaimer: This article provides general information about inverse-psoriasis and potential treatments. Medical advice and treatment should always be under a doctor’s supervision based on your specific case.